You Can't Be Healthy if You Mouth Breathe
- Sep 21, 2025
- 9 min read
Updated: Mar 31
It's impossible to be healthy if you mouth breathe. Our bodies are beautifully and wonderfully designed, and part of that perfect design is nasal breathing.
Immune Function & Inflammation
Our nose is designed to prepare the air for the lungs. The nose warms, filters, accelerates, humidifies, and cleans the air, which leads to efficient oxygen exchange in the lungs. The mouth does none of this, and actually reduces oxygen absorption. Nasal breathing also produces Nitric Oxide, an anti-inflammatory molecule that aids in immune function, lowers blood pressure, decreases the likelihood of blood clots, supports brain health, and balances hormones. Where as mouth breathing decreases immunity and causes inflammation throughout the body.
Think about hyperventilation. When you hyperventilate, you breathe rapidly through your mouth and don’t get proper oxygen exchange. Mouth breathing, whether during the day or at night, creates a similar effect. It keeps the body stuck in a constant fight-or-flight state, forcing your adrenal glands to stay on high alert around the clock.
Natural Palate Expansion
The tongue functions as a natural palate expander by pressing lightly and consistently against the roof of the mouth. This natural pressure influences the widening and shaping of the upper jaw, especially in growing children.

The proper resting position for the tongue is gently on the roof of the mouth, behind the front teeth.
When someone breathes through their mouth, the tongue naturally lowers to make room for airflow. Over time, this can create a habit of keeping the tongue in a low position and may contribute to a tongue-thrust swallowing pattern. This incorrect tongue position can cause a multitude of problems, like dental issues, speech difficulties, swallowing challenges, breathing problems, posture issues, etc.
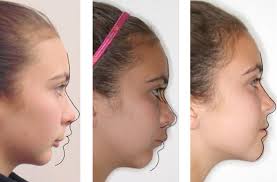
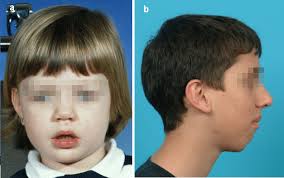
The Effects of Mouth Breathing on the Face

Click a photo to enlarge and scroll through gallery
Photo Sources:
Primate Studies
Two fascinating studies by Dr. Egil Harvold, published in the American Journal of Orthodontics and Dentofacial Orthopedics, observed young monkeys with plugged noses forcing them to adapt by mouth breathing.
This study found that ALL the monkeys who mouth breathed developed crooked teeth and poor jaws & facial development. Specifically, mouth breathing led to “a lowering of the chin, a steeper mandibular plane angle, and an increase in the gonial angle.” Their faces become long and narrow, with the jaw prominent and the chin recessed.

What Causes Mouth Breathing?
The underlying cause of mouth breathing will differ from person to person. If this is something you or your child struggle with, your first step should be an evaluation with an airway focused dentist. However, some common causes of mouth breathing include:
Oral restrictions (tongue ties)
Deviated septum
Nasap polyps
Habitual patterns
Mold exposure
Obesity
Underdeveloped jaws*
Narrow palate*
Sleep-disordered breathing*
Nasal congestion*
Allergies*
Food sensitivities*
Asthma*
Enlarged tonsils or adenoids*
*Which came first the chicken or the egg? These can be caused BY mouth-breathing, as well. For example: if there's an oral restriction that's preventing the tongue from resting in the proper position, this could lead to improper craniofacial development, which can lead to a narrow palate, which can lead to mouth breathing. Or if one is chronically mouth breathing, this can lead to inflamed and enlarged tonsils. This it why it's imperative to seek out an airway expert.
Mouth Breathing Consequences
Snoring, sleep apnea, upper airway resistance
Unrestful sleep
Frequent nighttime urination
Prolonged bedwetting
Chronic neck and shoulder pain
ADHD
Upper respiratory infections
Chapped, crust lips
Dry mouth
Inflamed gums and cavities
Oral disease
Speech difficulty / delayed speech
Teeth grinding
Headaches and migraines
Narrow palate
Crooked teeth
Vertigo/clumsiness
Agression/defiance
Allergies/asthma
Nightmares/night terrors
Recessed/stunted chin
Dark circles under the eyes
Daytime sleepiness
Chronic illness
Cardiovascular disease
Poor immune function
Poor gut health
Food sensitivities
Chronic inflammation
*Many of these are symptoms of a sleep breathing disorder, of which mouth breathing is a tell-tale sign
Mouth Breathing and Sleep Breathing Disorders
As mentioned, mouth breathing is a tell-tale sign of a sleep breathing disorder. A sleep breathing disorder is when someone has trouble breathing properly while they sleep (many throughout the day, as well). For kids, this can show up as snoring, restless sleep, mouth breathing, or even pauses in breathing during the night. Because their bodies are still growing, these interruptions can affect everything from brain development and behavior to growth and overall health.
When a child’s airway is too small or blocked, often due to underdeveloped jaws, enlarged tonsils/adenoids, or chronic allergies, it can make it harder for them to get enough oxygen while they sleep. Instead of the deep, restorative sleep their body needs, they wake up tired, cranky, and may struggle with focus, energy, or even mood during the day.
OSA vs UARS - the problem with sleep studies
If you have had a sleep study that came back negative for sleep apnea, but are experiencing mouth breathing or any of the above symptoms, and feel dismissed by your provider - it may be time to seek out a new, truly airway focused provider.
Obstructive Sleep Apnea (OSA) and Upper Airway Resistance Syndrome (UARS) are both sleep-related breathing issues, but they show up in different ways. OSA happens when the airway becomes blocked during sleep, causing pauses in breathing or very shallow breaths. This often leads to loud snoring, noticeable breathing pauses, drops in oxygen levels, and daytime sleepiness. It’s also linked to higher risks for things like high blood pressure, heart problems, and stroke. OSA is what is picked up during a sleep study.
UARS, on the other hand, is a bit different. Instead of full pauses in breathing, the airway becomes more narrow and resistant, making it harder to breathe smoothly. This doesn’t usually cause oxygen drops, but it does cause frequent sleep disruptions. People with UARS may not snore as loudly and may not seem “sleepy” during the day, but they often feel exhausted, unrefreshed, or struggle with insomnia-like symptoms.
Sleep studies do not typically pick up on UARS. If a study comes back negative for OSA, UARS could still be at large. If left untreated UARS will, most times, turn into sleep apnea. If a provider is not properly trained in airway disorders (most aren't), then this often goes overlooked.

Mouth Breathing and the Epidemic of Misdiagnosis
Mouth breathing is never normal, but what really raises concern is when it becomes chronic. If you have a cold and temporarily breathe through your mouth while your body fights off the infection, that’s not considered “normal," but once you return to healthy nasal breathing, there’s usually no lasting harm.
The real issue is when mouth breathing happens all day, every day, or even just consistently at night. That’s when it can start to impact development, airway health, and long-term wellbeing. After teaching 7th graders and working in the airway dentistry field for nearly a decade, I’ve seen countless health issues caused by mouth breathing, many of which parents weren’t aware of or were misdiagnosed.
Let's dive into a few of those now.
ADHD
This is probably the biggest one, along with other learning and behavioral difficulties. Mouth breathing is one of the tell-tale signs of a sleep breathing disorder. The AAPD recognizes that children with untreated obstructive sleep apnea may be inappropriately diagnosed with ADHD. Even the National Resource Center on ADHD acknowledges that ADHD may be associated with a state of increased sleepiness rather than hyperactivity.
So what's happening? Sometimes what looks like “ADHD” can actually be a sign of a sleep-related breathing problem. When a child (or adult) isn’t breathing properly at night, their sleep is fragmented and their body stays in a state of constant fatigue. To cope, the brain may ramp up activity to keep them awake, which can appear as hyperactivity or inattention.
Many of these individuals are diagnosed with ADHD and prescribed stimulant medications. While these drugs may help temporarily, they don’t address the underlying breathing issue, and in some cases, they can make overstimulation worse. Over time, higher doses may be needed, and the root cause remains untreated - not to mention medication unnecessarily being taken. Addressing the sleep and breathing problem directly is key, because untreated issues can lead to long-term health, behavioral, and cognitive consequences.
A side note on ADHD:
As a former educator, I also truly believe the restructuring of the eduction system has lead to diagnosis of ADHD that are absolute, excuse my language, bull crap. For boys, especially, the feminization of the school system is a huge problem. I highly recommend reading these books:
Why Gender Matters (great for parents and teachers of both genders)
Boys Adrift (if you have or teach boys)
Girls on the Edge (if you have or teach girls)
Enlarged Tonsils
Mouth breathing can create the perfection conditions for tonsil swelling. Breathing through the mouth dries out the throat and tonsils, making the tissues more prone to irritation and inflammation. It also bypasses the nose’s natural filtration system, exposing the throat to more dust, allergens, and bacteria, which can trigger immune responses and swelling. Over time, repeated infections and chronic irritation can lead to enlarged tonsils as the body tries to protect the airway.
There is research showing that expansion can minimize the size of tonsils and adenoids. This is a much more minimally invasive treatment than a tonsillectomy, which many times is just a band aid to a deeper root cause. With that being said, there is absolutely a time and a place for tonsillectomies, even if going through expansion or other treatments (typically these are pretty severe cases) - but this is why it's imperative to work with a qualified airway team.
Cavities
If you are on top of your child's oral hygiene and they are still experiencing chronic cavities, you may want to pay attention to their breathing. Dental health is influenced by the whole body, not just brushing and flossing. Chronic mouth breathing can dry out the mouth, reducing saliva flow, which helps neutralize acids, remineralize teeth, and wash away harmful bacteria. Without enough saliva, the oral environment becomes more acidic and favors acid-producing anaerobic bacteria - conditions that routine brushing alone can’t fully control.
Chronic Allergies
Chronic mouth breathing and chronic allergies are often linked in a feedback loop, with each potentially contributing to the other. Mouth breathing bypasses the nose, which normally filters dust, pollen, and other environmental irritants, allowing more allergens to enter the airway and triggering inflammation. Over time, this can worsen or prolong allergy symptoms. Conversely, chronic allergies (from causes such as environmental pollution, dust, mold, pollen, or pet dander) can inflame nasal passages and sinuses, making it harder to breathe through the nose and encouraging mouth breathing. It’s often hard to say which comes first because habitual mouth breathing can exacerbate allergies, while persistent allergic inflammation can reinforce mouth breathing, creating a cycle that can be difficult to break.
Food Sensitivity
Chronic mouth breathing can contribute to food sensitivities, though usually indirectly. Breathing through the mouth dries out saliva, which is essential for proper digestion and neutralizing acids. It can also promote oral bacterial imbalances and contribute to systemic inflammation, both of which may affect the immune system and increase reactivity to certain foods. Additionally, mouth breathing can alter chewing and swallowing patterns, making digestion less efficient and potentially heightening sensitivity to certain foods over time.
On the other hand, however, if the food sensitivity starts first that can then lead to mouth breathing by causing inflammation and congestion in the nasal passages and throat. When the body reacts to a triggering food, it can cause swelling in the sinuses or nasal passages, partially blocking airflow through the nose. This congestion often forces the individual to breathe through the mouth to get enough air. Additionally, increased mucus production and post-nasal drip from food sensitivities can irritate the throat, making nasal breathing uncomfortable and reinforcing the habit of mouth breathing over time.
Again, which came first - the chicken or the egg?
Mouth Breathing Interventions
Treatment will vary depending on age and severity. If caught early during childhood, the treatment is often much more simple. Early correction for optimal child development will typically involve a TEAM approach of an airway centered & trained dentist, an ENT specialist, speech/myofunctional therapist, body worker, and possibly orthodontist.
A common treatment is palatal expansion. Palatal expansion is a process that gently widens the roof of the mouth. Using a custom-made appliance, your child’s upper jaw is gradually expanded to support healthy facial growth. This increased width creates more room for permanent teeth, can help open the airway to encourage nasal breathing, and may reduce the need for extensive orthodontics later on.
Dr. Nora Zaghi has lots of detailed, parent-friendly information on palatal expansion.
Browse a list of providers by state here.

The Relationship between Nocturnal Enuresis and Obstructive Sleep Apnea in Children
Prevalence of upper respiratory tract infections in habitually snoring and mouth breathing children
The AAPD recognizes that children with untreated obstructive sleep apnea may be inappropriately diagnosed with ADHD.
Even the National Resource Center on ADHD acknowledges that ADHD may be associated with a state of increased sleepiness rather than hyperactivity.
Due to the clinically significant relationship between adenotonsillar hypertrophy, OSA, and ADHD, adenotonsillectomy should be considered as a treatment option for ADHD in pediatric OSA patients
A Randomized Trial of Adenotonsillectomy for Childhood Sleep Apnea
There is research showing that expansion can minimize the size of tonsils and adenoids.










Comments